Heart Anatomy: chambers, valves and vessels
Heart chambers and associated great vessels
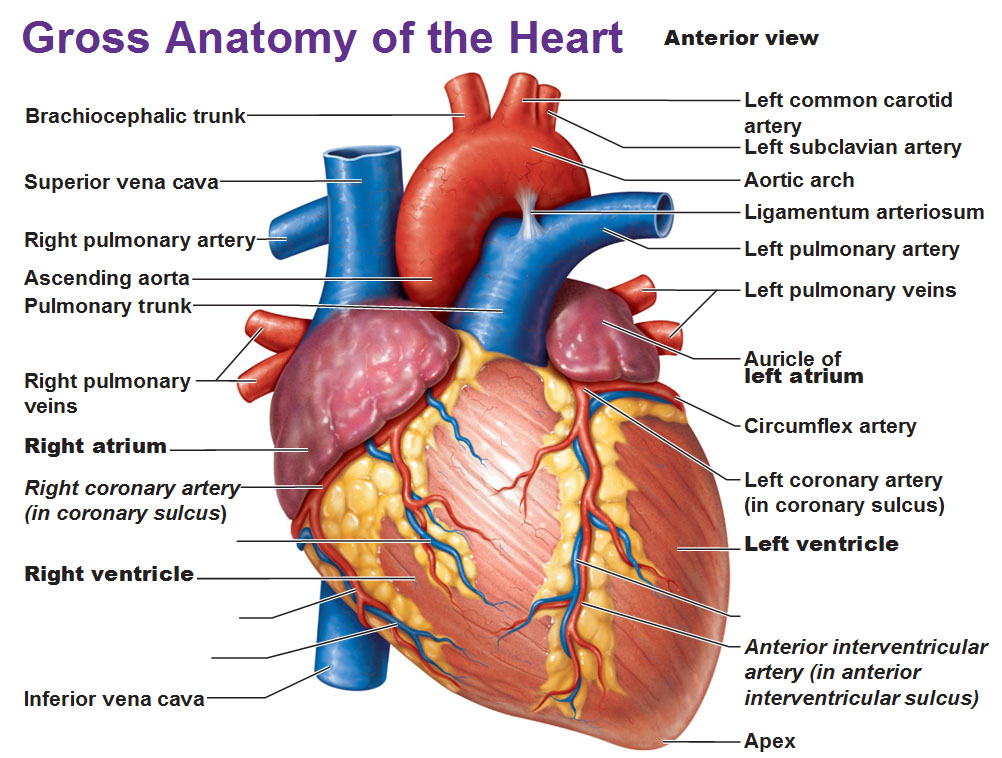
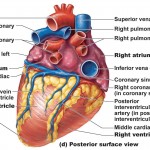
The heart has four chambers – two superior atria and two inferior ventricles. The internal partition that divides the heart longitudinally is called the interatrial septum where it separates the atria, and the interventricular septum where is separates the ventricles. The right ventricle forms most of the anterior surface of the heart, while the left ventricle forms the heart apex.
Two grooves on the heart surface indicate the boundaries of its four chambers and carry the blood vessels supplying the myocardium. The coronary sulcus, also called the atrioventricular groove, encircles the junction of the atria and ventricles like a crown. The anterior interventricular sulcus cradles the anterior interventricular artery and also marks the anterior position of the septum, where the right and left ventricles separate. It continues as the posterior interventricular sulcus, which marks a similar position on the poseroinferior surface.
Atria: The Receiving Chambers
The only surface feature on each atrium is a small, wrinkled , appendage called an auricle. Auricles increase atria volume slightly. Internally, the
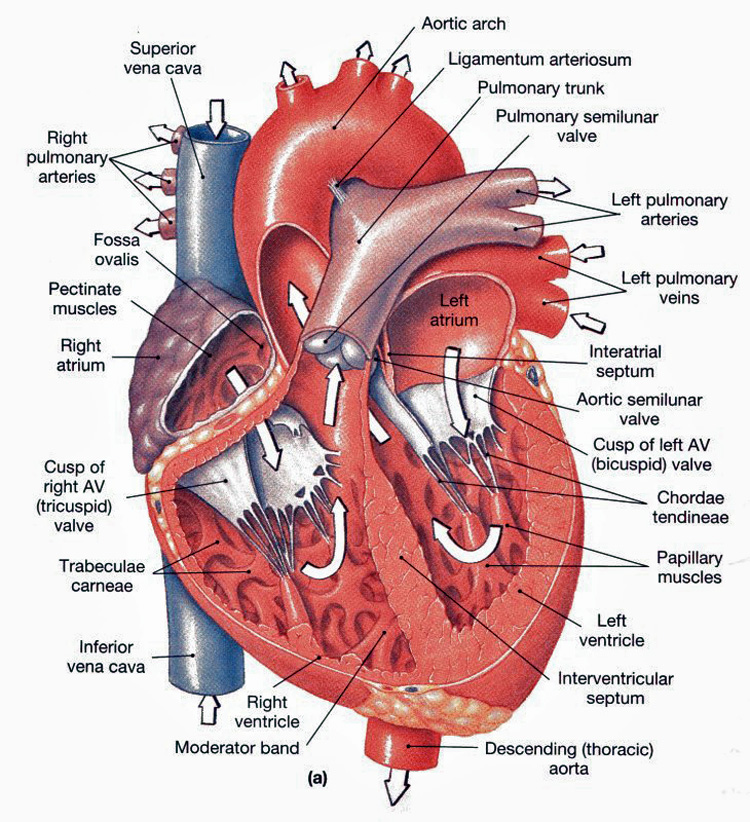
right atrium has two basic parts: a smooth posterior and an anterior portion in which bundles of muscle tissue form ridges in the walls. The muscle bundles are called pectinate muscles because they look like the teeth of a comb. The right atrium’s posterior and anterior region are separated by a C-shaped ridge called the crista terminalis.
In contrast, the left atrium is almost entirely smooth and pectinate muscles are only found in the auricle. The interatrial septum contains a shallow depression called the fossa ovalis. The fossa ovalis marks the spot where an opening, the foramen ovale, existed in the fetal heart. The opening closes after birth.
The atria are receiving chambers for blood returning to the heart from circulation. Atria are relatively small, thin-walled chambers because they only need to contract minimally to push blood into the ventricles. In reality, the contribute little to propulsion and pumping activity of the heart. Blood enters the right atrium through three veins:
- The superior vena cava returns blood from body regions superior to the diaphragm.
- The inferior vena cava returns blood from body areas below the diaphragm.
- The coronary sinus collects blood draining from the myocardium.
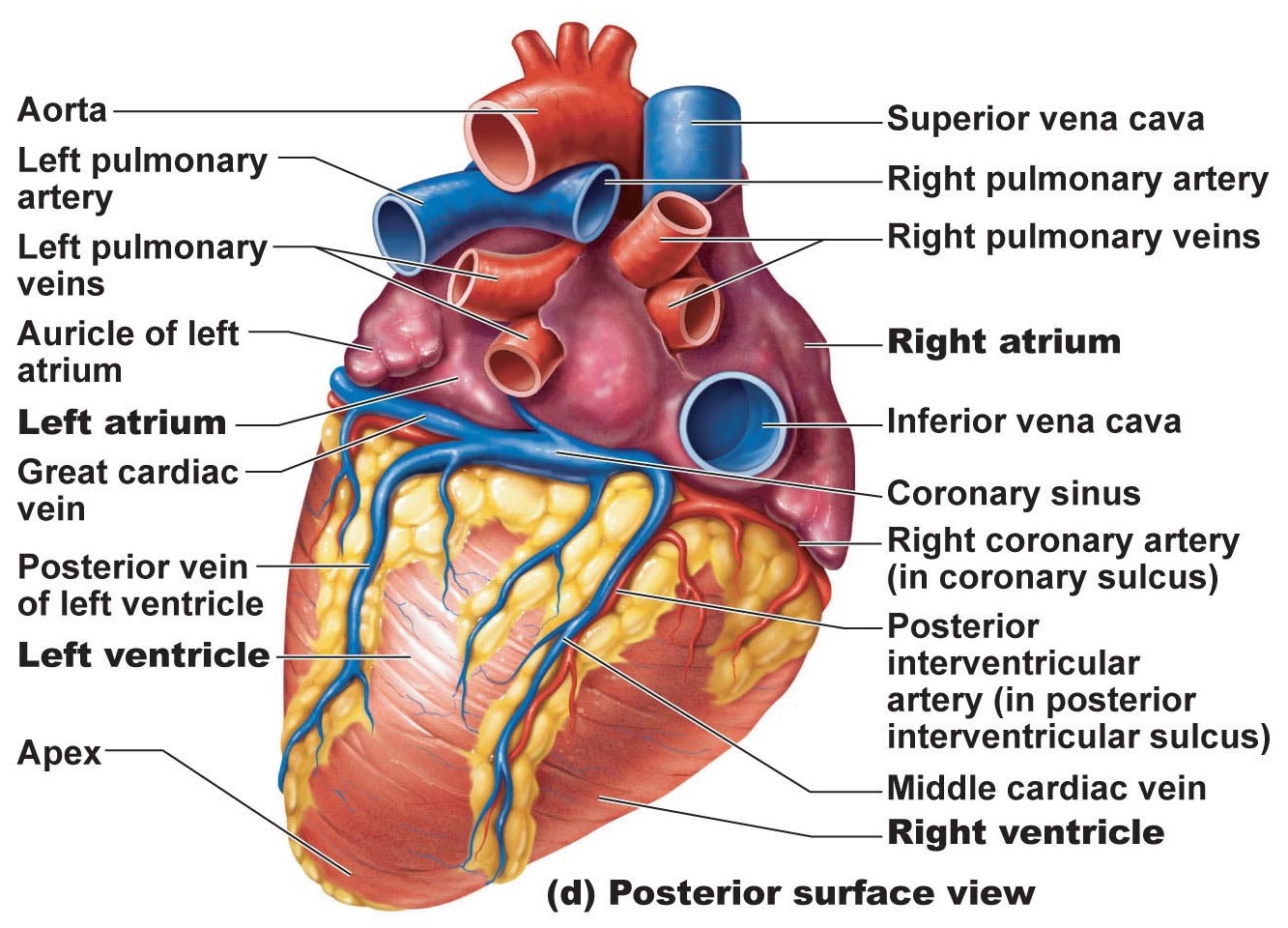
Four pulmonary veins enter the left atrium. These veins, which transport blood from the lungs back to the heart, are best seen in a posterior view.
Ventricles: Discharging chambers
The ventricles make up most of the volume of the heart. The right ventricle forms most of the heart’s anterior surface and the left ventricle forms most of the poseroinferior surface. Irregular ridges of muscle called trabeculae carneae mark the internal walls of the ventricular chambers. Another group of muscle bundles called papillary muscles project into the ventricular cavity and play a role in valve function. The ventricles are the discharging chambers, the actual pumps of the heart. Their walls are larger than atrial walls and when they contract, they propel blood out of the heart into circulation. The right ventricle pumps blood into the pulmonary trunk, which sends the blood to the lungs where gas exchange occurs. The left ventricle ejects blood into the aorta, the largest artery in the body.
Heart Valves
Blood flows through the heart in one direction: from the atria to the ventricles and out the great arteries leaving the superior aspect of the heart. Four valves enforce the one-way traffic. They open and close in response to differences in blood pressure.
Atrioventricular (AV) Valves
There are two atrioventricular (AV) valves. One is located at each atrial-ventricular junction and they prevent backflow into the atria when the ventricles contract.
- The right AV valve, or tricuspid valve, has three flexible cusps.
- The left AV valve has two cusps. It’s called the mitral valve and is sometimes called the bicuspid valve.
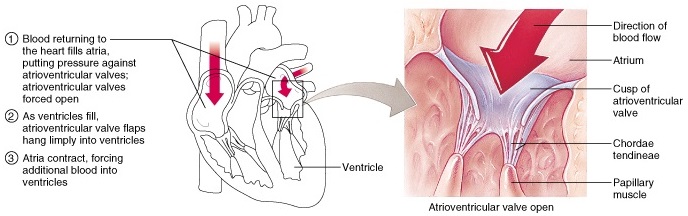
Attached to each AV valve flap are collagen chords called chordae tedineae, which anchor the cusps to the papillary muscles. When the heart is completely relaxed, the AV valves flaps hang limp and blood flows into the atria and then through the open AV valve flaps into the ventricles. When the ventricles contract, compressing the blood into their chambers, the pressure rises forcing the blood superiorly against the valve flaps. Because of this, the flap edges meet and successfully close the valve.
Chordae tendineae and papillary muscles serve as wires that anchor the valve flaps in their closed position. If the cusps weren’t anchored, they would be blown into the atria the same way an umbrella is blown inside out by the wind. The papillary muscles contract and take up the slack on the chordae tendineae when contractions forcefully hurl blood against the AV valve flaps.
Semilunar (SL) Valves
The aortic and pulmo
nary (semilunar, SL) valves guard the bases of the largest arteries stemming from the ventricles and prevent backflow into the associ
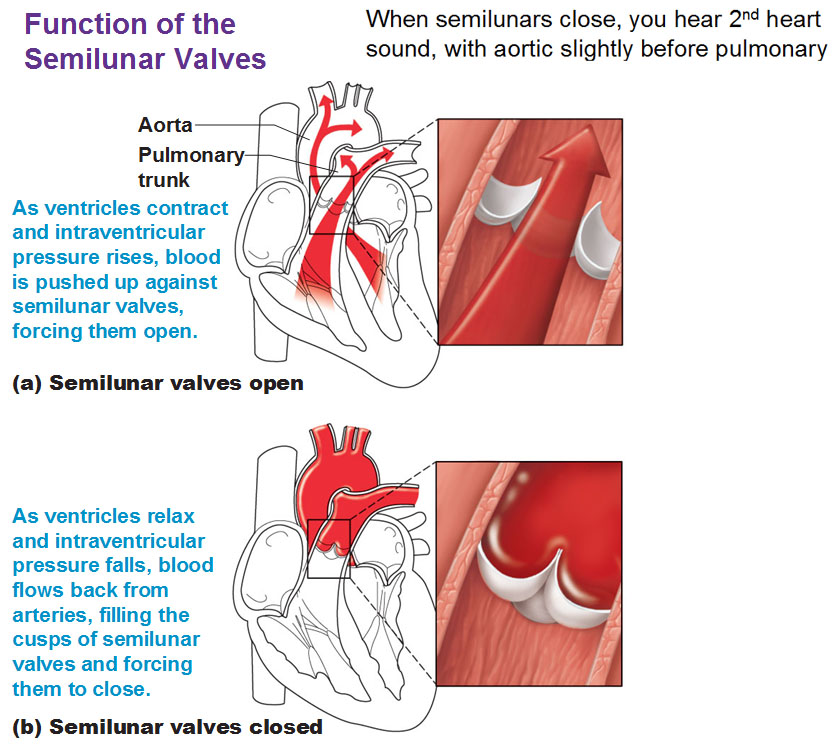
ated ventricles. Each valve has three cusps, shaped like a crescent moon. The semilunar valves open and close in response to differences in pressure. When the ventricles contract and pressure rises higher than the pressure in the aorta and pulmonary trunk, the valves are forced open and their cusps flatten while blood rushes in. When
the ventricles relax and bloodflows back toward the heart, the cusps become full and the valves close. Heart valves – like any mechanical pump, can function with leaks, but if a valve is badly damaged it can greatly reduce cardiac function. A damaged valve forces the heart to re-pump blood over and over because the valve doesn’t close properly and backflow occurs. Because of this, the heart will weaken over time due to overwork.
Sometimes, valves can be replaced with a mechanical valve, or even an animal valve (pig, cow) if it’s chemically treated to prevent rejection. Cryopreserved heart valves from
human cadavers have been used too. Currently, scientists are working on developing heart valves engineered from a patients own cells.
Related Posts
Category: Cardiovascular



Thanks for very clear illustrations.